Bariatric Surgery
Bariatric Surgery Dietetic Services
Bariatric surgery represents a form of surgical treatment and management of obesity.
In Australia, two primary types of bariatric surgery are performed: sleeve gastrectomy and gastric bypass.
- Sleeve gastrectomy involves removing a portion of the stomach, resulting in a smaller, sleeve-shaped stomach, providing restriction to food intake.
- Gastric bypass entails creating a small pouch at the top of the stomach, connecting it directly to the small intestine, effectively bypassing the rest of the stomach.
While both procedures aid in weight loss, gastric bypass is particularly recommended for individuals with diabetes due to its favourable impact on blood sugar control, and for those with reflux issues, as it mitigates the risk of worsening symptoms.
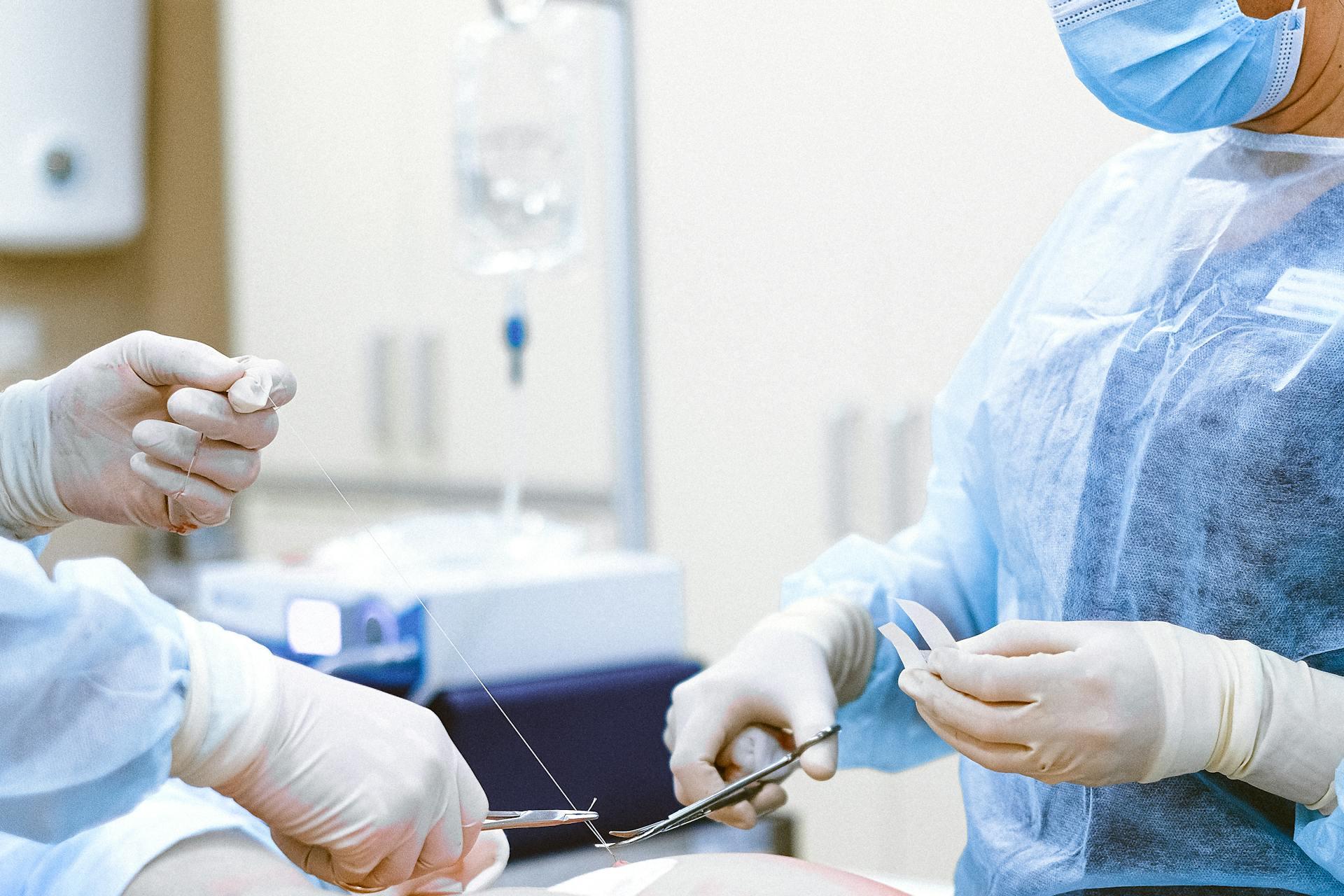
Role of Dietitians in Bariatric Surgery
Collaborating with bariatric surgeons, Dietitians play a crucial role in the pre- and post-operative phases. Patients typically consult with a Dietitian at least twice before surgery. Initially, a nutrition assessment is conducted to address eating behaviours and establish dietary habits conducive to long-term health.
Patients are guided through a Very Low-Calorie Diet (VLCD) to reduce the size of the liver, which can make surgery safer by lowering the risk of complications. During periods of calorie restriction or fasting, the liver’s glycogen stores are depleted to provide glucose for energy.
Pre-surgery, the VLCD is a short-term and low-carbohydrate diet (for example, 800 calories/50g carbs per day) aimed at preparing the body for the procedure.
Post-surgery, patients transition through a liquid-only diet, followed by pureed and soft food textures over four to six weeks. The dietary focus post-surgery revolves around ensuring adequate nutrient intake while respecting the stomach’s healing process.
The caring Dietitians at Healthcare on Collins provide this service to people throughout Melbourne.

Understanding Bariatric Surgery
Bariatric surgery is not a cosmetic procedure but a medical intervention. Bariatric surgery is typically considered for individuals who have severe obesity, possibly combined with comorbidities such as sleep apnea, diabetes or high blood pressure.
Unlike cosmetic procedures like liposuction, which targets fat removal, bariatric surgery addresses underlying metabolic issues.

Multidisciplinary Care & Healthcare Pathway
Having a supportive General Practitioner (GP) to oversee blood tests and provide ongoing care is essential.
Additionally, engagement with an Exercise Physiologist post-surgery aids in recovery and minimises muscle atrophy.
Psychological support, both pre-and post-surgery, is also recommended to address potential eating disorders or disordered eating behaviors.
Appointment Information
Appointment Schedule
Patients generally attend two pre-operative appointments, followed by consultations at six weeks, six months, and twelve months post-surgery. However, additional appointments can be scheduled as needed for ongoing support and monitoring.
Long-Term Management
Bariatric surgery, such as gastric bypass or sleeve gastrectomy, alters the anatomy of the digestive system, which can affect the body’s ability to absorb certain nutrients efficiently.
Following surgery, lifelong adherence to a specific bariatric multivitamin regimen is essential to address potential nutrient deficiencies. While these vitamins may not be readily available at local pharmacies, patients are advised to obtain them from hospital-affiliated pharmacies or online sources.


Why Choose Healthcare on Collins?
While specific accreditation in bariatric surgery is not mandatory for Dietitians, tailored professional development is essential to provide optimal care.
The focus of dietitians is on fostering healthy relationships with food and ensuring long-term well-being, rather than simply prescribing diets.
Your surgeon or GP can refer you to a Dietitian with suitable qualifications to support your needs.
Contact Healthcare on Collins for Dietitian Support
Through collaborative efforts between patients, healthcare professionals, and Dietitians, individuals can achieve sustainable weight loss and improved overall health and well-being.
You can trust in Healthcare on Collins as a professional provider of bariatric surgery supports, please use the contact page to get started.
Call Us
(03) 9650 4284

FAQ
Why do bariatric surgery patients often need supplements like iron, vitamin D, zinc, and vitamin A?
Bariatric surgery alters the digestive system’s anatomy, affecting the absorption of essential nutrients. Here’s why these supplements are commonly required:
- Iron: Iron deficiency is common due to changes in the intestine that affect iron absorption, impacting red blood cell production and energy levels.
- Vitamin D: Surgery can hinder the absorption of vitamin D, crucial for calcium absorption, bone health, and immune function.
- Zinc: Absorption of zinc, important for immune function and wound healing, may also be affected.
- Vitamin A: Some procedures reduce the absorption of fat-soluble vitamins like vitamin A, vital for vision, immune function, and skin health.
Regular supplementation and monitoring by healthcare professionals are essential post-surgery to prevent deficiencies and maintain overall health.
